Treatment
Most of the information in this section pertains to intrinsic brain tumours such as Gliomas or metastases. For tumours such as meningiomas, acoustic neuromas and pituitary adenomas even though general principles of intracranial surgery apply, there will be specific issues pertaining to these tumours that will be detailed in the relevant sections. The first treatment for most brain tumours is either surgery to remove the tumour or a biopsy to obtain a small sample of tumour. The tumour tissue that is removed is used to determine the exact type of tumour. Find out more about surgery for suspected brain tumours here:
There are several types of equipment available to the neurosurgeon. Specialised equipment is used to accurately localise the tumour within the brain and to track the margins of normal and abnormal tissue. This is similar to a satnav while driving, where the position of your car is shown relative to the street map. This is known as Image guidance (or Neuro navigation) and it increases safety and accuracy of tumour resection. Ultrasonic aspirators can be used to break up and suck out the tumour. High-powered microscopes may be used to better see the tumour tissue and surrounding nerves and blood vessels. Because the tentacle-like cells of an astrocytoma grow into the surrounding tissue, complete resection of these tumours is difficult to achieve without also removing normal brain tissue. Therefore a compromise has to be made between removing tumour tissue and preserving normal tissue. At surgery visibly abnormal looking tissue is removed. If the image guidance equipment shows that what looks visibly like normal brain could also represent abnormal tumour, then that area is also removed if it is felt by the surgeon that it will not lead to any compromise in neurological function. If the abnormal looking area on image guidance is an area that is vital for important bodily functions, then it is left intact, and treated non surgically depending on the type of tumour. Partial removal can help decrease symptoms and confirm the type of tumour.









 Weight loss surgery isn’t a ‘quick fix’ or a certainty that you will lose weight. It is a tool to help your weight loss. Successful weight loss will be entirely down to you making good dietary choices and being as physically active as possible. In the initial period after surgery you will only be able to eat very small portions and will probably not feel hungry. Both these factors may change with time.
Weight loss surgery isn’t a ‘quick fix’ or a certainty that you will lose weight. It is a tool to help your weight loss. Successful weight loss will be entirely down to you making good dietary choices and being as physically active as possible. In the initial period after surgery you will only be able to eat very small portions and will probably not feel hungry. Both these factors may change with time.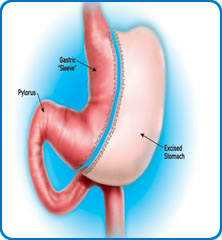 This operation involves removing approximately 80% of the stomach, leaving a thin tube or sleeve (about the width of your thumb) which holds about 50-100mL of fluid (about ½ cup of tea). The ‘gut’ or digestive tract remains intact below the stomach. It works by restricting the volume of food you can eat. It also removes some stomach cells that produce a hormone that controls hunger, so patients often don’t feel as hungry afterwards. This has positive effects on diabetes and often patients can stop their medication after surgery. The operation takes about one hour and the hospital stay is 1 day.
This operation involves removing approximately 80% of the stomach, leaving a thin tube or sleeve (about the width of your thumb) which holds about 50-100mL of fluid (about ½ cup of tea). The ‘gut’ or digestive tract remains intact below the stomach. It works by restricting the volume of food you can eat. It also removes some stomach cells that produce a hormone that controls hunger, so patients often don’t feel as hungry afterwards. This has positive effects on diabetes and often patients can stop their medication after surgery. The operation takes about one hour and the hospital stay is 1 day.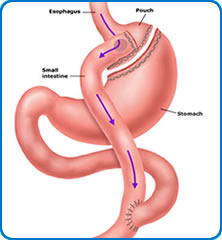 The gastric bypass is a more complicated procedure and involves the creation of a small pouch at the top of the stomach with staples. The remaining stomach stays in place. A section of intestine is ‘plumbed’ into this pouch so that the food bypasses the rest of the stomach and enters the intestine lower down. There are therefore two joins of the intestine inside. It works by limiting the amount you can eat at each mealtime but also by altering the hormone levels produced by the gut to improve diabetes and make you less hungry. The operation takes about one hour and the hospital stay is usually 1 day.
The gastric bypass is a more complicated procedure and involves the creation of a small pouch at the top of the stomach with staples. The remaining stomach stays in place. A section of intestine is ‘plumbed’ into this pouch so that the food bypasses the rest of the stomach and enters the intestine lower down. There are therefore two joins of the intestine inside. It works by limiting the amount you can eat at each mealtime but also by altering the hormone levels produced by the gut to improve diabetes and make you less hungry. The operation takes about one hour and the hospital stay is usually 1 day.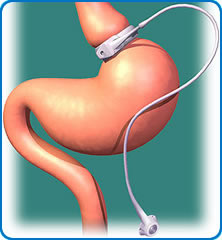 The band consists of a silicone tube with a balloon device on one end and an inflation port on the other. It is fitted at the very top of the stomach with a small ‘inflation port’ underneath the skin on the left hand side of the tummy. It works by dimming the appetite and slowing your eating down. This, together with behavioral changes and mindful eating aims to result in lessening the volume of food you eat. The tightness of the band can be adjusted by altering the volume of liquid within the band by a simple injection into the port. The operation takes less than an hour, although there is time taken in both putting you to sleep and waking you up afterwards so the overall time away from the ward is three to four hours.
The band consists of a silicone tube with a balloon device on one end and an inflation port on the other. It is fitted at the very top of the stomach with a small ‘inflation port’ underneath the skin on the left hand side of the tummy. It works by dimming the appetite and slowing your eating down. This, together with behavioral changes and mindful eating aims to result in lessening the volume of food you eat. The tightness of the band can be adjusted by altering the volume of liquid within the band by a simple injection into the port. The operation takes less than an hour, although there is time taken in both putting you to sleep and waking you up afterwards so the overall time away from the ward is three to four hours.







