Pelvic floor exercises for men
This page contains information for patients about pelvic floor exercises for men.
Where are my pelvic floor muscles?
They are the layer of muscles that extend from your pubic bone at the front of your pelvis to your tail bone (coccyx) at the back of your pelvis. They are the the muscular support at base of your pelvis.
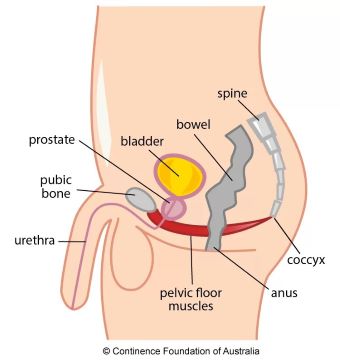
What are the functions of your pelvic floor?
- Bladder control.
- Bowel control.
- Sexual function.
- Stabilises the pelvis.
- Supports the pelvic organs.
Possible risk factors leading to pelvic floor weakness:
- Prostate or pelvic surgery (e.g. prostatectomy).
- Radiation to the pelvis.
- Straining to poo due to chronic constipation.
- Certain conditions such as MS, strokes, or uncontrolled diabetes.
- Being overweight.
- Chronic coughs.
- Injury to the perineum.
What are the symptoms of pelvic floor weakness in men?
Many men experience weakness of the pelvic floor. If this happens you may have a variety of symptoms including:
- Leaking urine during activity, for example when you sneeze, cough or laugh (known as stress urinary incontinence).
- A need to go to the toilet often during the day or night (known as frequency or nocturia, respectively).
- An urgent need to visit the toilet and leaking before you get there (known as urgency incontinence).
- You are unable to control the passing of wind or stool from your back passage.
- Erectile dysfunction (the pelvic floor helps you maintain erections).
- Post micturition dribble (leaking urine immediately after you have finished passing urine).
Why should I do pelvic floor exercises?
The pelvic floor muscles can be strengthened to increase the support of the pelvic organs. This can improve bladder and bowel control and can reduce/cure leakage of urine. It may also improve your ability to maintain an erection.
Identifying the pelvic floor muscles
It’s important to know where the pelvic floor muscles are, so that you’re sure you’re exercising the correct muscles. To identify the pelvic floor muscles, tighten your back passage as if you’re trying to stop yourself passing wind; at the same time, imagine you’re trying to stop yourself passing urine.
You should have a sense of squeezing, pulling the back passage up and in. You may see the base of your penis retract slightly in your body and your testicles rise a little. Do not tighten your thighs or buttocks and do not hold your breath. After contracting it is important to feel the muscles relaxing and softening as you let go.
How do I do pelvic floor exercises?
You can exercise your pelvic floor anywhere and anytime. They can be performed lying, sitting or standing but to start with it may be easier to do the exercises sitting down. Make sure you’ve found the correct muscles and know how it should feel when you tighten them before trying these exercises.
There are two types of exercises, slow and fast, it is important you do both:
Exercise 1: slow pull-ups
- Take a breath in.
- On the breath out, tighten the pelvic floor muscles.
- Return to normal breathing but continue to tighten for your length of hold, relax, and feel the muscle let go.
- Rest for 5 seconds.
- Repeat this 5 times.
As it gets easier, gradually increase length of hold and number of repetitions, aiming for 10 seconds.
Exercise 2: fast pull-ups
- Tighten the pelvic floor muscles quickly and then let go straight away.
- Repeat this 10 times – approximately 1 contraction per second.
You may find that the muscles are weak initially and that it takes a lot of concentration to exercise them, but this should improve with time
Do not practice stopping the flow of urine midstream as this may interfere with the normal process of emptying your bladder.
How often should I do my exercises?
Do exercises 1 and 2 during each session. As soon as you can, increase to 10 slow and 10 fast pull-ups.
Aim to repeat these 3 times each day, so in total you will be doing 30 slow and 30 fast pull-ups a day.
It will take up to 3-6 months of regular exercise to increase the strength in your pelvic floor muscles and hopefully reduce your symptoms.
As your muscles get stronger you may progress to doing the exercises standing up.
To help remind you to do your exercises daily try to combine them with an everyday activity, for example, when brushing your teeth, and after breakfast, lunch, and dinner.
You can also download an app called Squeezy which is recommended by the NHS. It will send you reminders to do the exercises and you can personalise the programme to suit you.
How long should I continue with the exercises?
Once your symptoms have improved, continue with these exercises once daily for the rest of your life to keep these muscles fit and healthy (e.g., 10 slow and 10 fast pull-ups daily).
Additional tips
- Being overweight can weaken the pelvic floor muscles so it is important to maintain a healthy BMI.
- You may want to try sitting in the correct toilet position to help with constipation like in the image below. (This is sat on a toilet with feet on a foot rest, knees higher than your hips, lean forward with your elbows onto your knees. Bulge out your abdomen and straighten your spine).
- You should try to drink 6-8 cups of fluid a day.
- Caffeinated drinks, alcohol, acidic drinks (fruit juices) and fizzy drink can irritate your bladder and cause urgency; we suggest avoiding these.
- Tighten the pelvic floor muscles before lifting anything heavy or if you are going to sneeze or cough.
- If you have urgency, contract your pelvic floor muscles when you have the desire to empty your bladder and only move when the desire has passed.
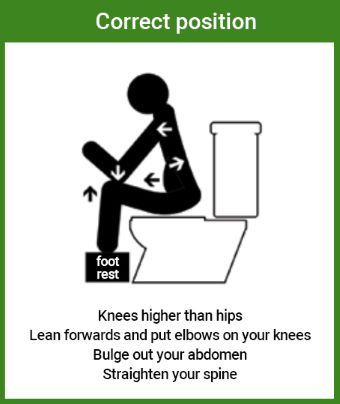
Image courtesty of Bladder and Bowel Community:
www.bladderandbowel.org/help-information/resources/toilet-positions/
© North Bristol NHS Trust. This edition published May 2024. Review due May 2027. NBT002673.