This page is for patients diagnosed as having a rib or chest injury.
Chest injuries are extremely common following blunt and penetrating trauma. They can vary in severity from minor bruising or an isolated rib fracture, to severe crush injuries. These can cause multiple fractures and bleeding which result in pain and breathing problems.
Common causes of rib injury include motor vehicle accidents, falls, and assaults. Treatment aims to relieve pain allowing you to perform normal tasks while the injury heals.
The majority of chest injuries are treated without requiring an operation, but a chest drain may need to be inserted.
Occasionally with severe injuries the ribs may have to be fixed. This requires an operation that is performed under general anaesthetic (you will be asleep).
If you follow the advice given to you in this booklet and by the healthcare professionals on the ward, you should find your chest injury much easier to understand and manage.
Types of injury
Your clinician will let you know which injury type you have.
Rib fractures
A rib fracture is a break in a rib bone. Bruising of the surrounding muscles and ligaments often occurs with these rib fractures. The lungs and other organs underneath the ribs may also be injured.
Flail chest
A flail chest occurs when a segment (part) of the rib cage is separated from the surrounding structures. This is usually defined as at least two fractures per rib, in at least two ribs.
Sternal fracture
A sternal fracture is a fracture of the sternum (the breastbone), located in the centre of the chest.
Pneumothorax
A pneumothorax is a collection of air between the lung and chest wall that causes part or all of a lung to collapse.
Haemothorax
A haemothorax is a collection of blood between the lung and chest wall which may be caused by blunt or penetrating injury.
Lung contusion
A lung contusion is bruising or bleeding of the lung tissue that may cause pain and trouble breathing. It is a common lung injury after blunt trauma to the chest wall.
The chest
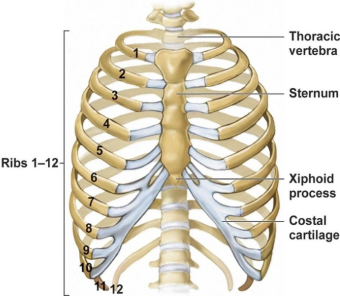
The ribcage supports the upper body, protects internal organs, including the heart and lungs, and assists with breathing.
Rib injuries include bruises, torn cartilage and bone fractures.
Symptoms of chest trauma
- Pain at the injury site.
- Pain when the ribcage moves. For example with movement, when you take a deep breath or when you cough, sneeze or laugh.
- Breathing difficulties.
- Coughing up blood or discoloured sputum.
- Increased temperature.
Treatment of chest injuries
- Pain relief.
- Oxygen therapy.
- Early mobilisation.
- Physiotherapy.
- Chest drain(s).
Very occasionally surgery is required to stabilise the fractures. In severe cases intensive care treatment is also required. If this is needed your doctor will discuss it with you/your family.
Complications
Possible complications of chest trauma include:
- Pain.
- Pneumothorax/haemothorax (definitions above).
- Chest infection – to avoid this it is important to ensure your pain relief is enough so you are able to take deep breaths, cough, and mobilise.
Pain management
- The most important treatment with chest trauma is to have good pain relief.
- Take regular pain relief so you are able to deep breathe, cough, and mobilise – these are vital for you to do as they aid your recovery and help prevent complications such a chest infection.
- Inform your nurse and doctors if you feel your pain relief isn’t adequate.
- Take the recommended pain relief and/or anti-inflammatory tablets; these will improve your healing time.
Lidocaine plasters for rib fractures
Lidocaine is a local anaesthetic which works by diffusing into the skin, causing numbness and relieving pain at the site of the rib fractures.
You may have been given lidocaine plasters to treat pain from rib fractures and to enable you to deep breathe and cough more easily.
Prior to using the plaster any allergies should be discussed with your healthcare professional to ensure this treatment is safe for you.
Between one and three plasters will be used depending on your rib injuries. The plaster/s must be applied to dry skin with no cuts or sores. Any hairs over the affected area may be trimmed with scissors (not shaved). Do not apply cream or lotion to the area as the plaster may not stick. If you have had a recent bath or shower, wait until the skin cools before sticking the plaster on. Try not to then get the plaster wet.
Lidocaine plasters must only be left in place for 12 hours, then they must be removed for a 12 hour break. For example, your plasters may be applied at 9am and removed at 9pm so that you have a break from them overnight.
Local anaesthetic nerve blocks (epidural, paravertebral or “fascial plane” blocks)
These provide effective pain relief through an injection of local anaesthetic to help numb the injured area. A very small, sterile plastic tube may be inserted to infuse local anaesthetic and help reduce your pain for several days. Anaesthetists perform these blocks and will explain everything to you including any risks.
Chest drains
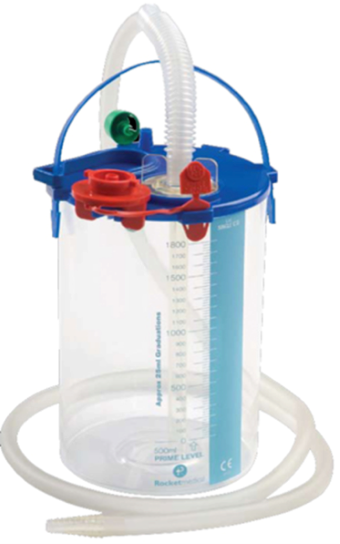
If you have a pneumothorax or haemothorax you may need to have a chest drain inserted. If this is required your doctor will discuss it with you and explain the procedure.
A chest drain is a sterile soft plastic tube that is inserted into the space between the lung and the chest wall. It is used to drain air (pneumothorax) or blood (haemothorax).
If you have a chest drain some important things to know are:
- You may see air bubbling out through the drainage bottle or fluid draining. This is expected and will be monitored.
- You must keep the drainage bottle below the point the drain enters your chest. Usually it is placed on the floor. It is also essential that the bottle is kept upright.
- The drain can come out if pulled or twisted so try to be careful when moving. If the drain does come out tell someone straight away.
- The drain may cause discomfort, but is unusual to cause significant pain. If it is painful inform your nurse and ask for painkillers.
Physiotherapy and breathing exercises
Breathing exercises
Start in a comfortable position, ideally sitting upright in the bed or chair with your shoulders relaxed.
- Take a long, slow, deep breath in, as much as possible.
- Hold this breath for three seconds.
- Slowly breathe out.
- Take three more deep breaths in the same way.
- Return to breathing normally.
- Try to repeat once every hour.
Coughing
The breathing exercise should be followed by a cough. It is very important to cough effectively after a chest injury so that you can clear any sputum promptly and help prevent a chest infection.
Discomfort may be reduced by using a folded towel or pillow to support your chest while coughing.
If you feel that you are unable to clear your chest effectively or are concerned about an excessive amount (too much) of sputum, please inform your nurse who will refer you to the respiratory physiotherapist.
Repeat the breathing exercises and coughing at regular intervals for the first few days following your injury. They may be discontinued (stopped) when you are walking independently and your chest is clear.
Early mobilisation
You will be assisted by the nursing staff or physiotherapist to mobilise (move around) as soon as possible after your injury. It is essential your pain relief is adequate to enable you to do this.
What to do once you are discharged from hospital?
It is very important to continue to take regular pain relief as prescribed.
Once you have been discharged from hospital make an appointment to see your GP within three days.
Your GP may order a follow up chest X-ray and monitor your broken rib(s).
You need to tell your GP:
- If you are feeling more unwell since going home.
- If you develop a fever.
- If your pain medication is not working.
- If you are not able to deep breathe or cough.
- If you are a smoker.
- If you are constipated from pain medication.
Take your hospital discharge summary with you. This summary tells the GP what has happened, tests done and what should happen with your care.
You should seek medical advice immediately from either your GP or emergency department if you have any of the following symptoms after discharge:
- Sudden onset of chest pain.
- Difficulty breathing.
- Shortness of breath.
- Uncontrolled pain.
© North Bristol NHS Trust. This edition published April 2024. Review due April 2027. NBT002945
Support your local hospital charity

See the impact we make across our hospitals and how you can be a part of it.

