Overview
Over time your Parkinson’s treatment may stop working well enough to control your symptoms. At this point other options may be considered, such as surgery or medications given as infusions or injections.
These treatments don’t cure Parkinson’s, but can help improve movement problems and quality of life, particularly for certain types of problems like:
- Motor fluctuations: this is where your tablets don’t last between doses or cause involuntary movements (known as dyskinesias).
- Tremors which are causing problems.
There are a range of different advanced treatments available. These are called device-assisted therapies (DAT). These treatments aim to provide steady flow of dopamine to help improve motor symptoms.
DAT are not suitable for everyone with Parkinson’s. The following information gives you an overview of the options. You can discuss them further with your Parkinson’s specialist or if you are referred to a specialist DAT clinic.
Currently there are five different DAT available for Parkinson’s:
- Deep brain stimulation (DBS).
- Apomorphine - an injection or infusion of a dopamine agonist under the skin.
- Duodopa - Levodopa-Carbidopa Intestinal Gel (LCIG).
- Lecigon - Levodopa-Carbidopa-Entacapone Intestinal Gel (LECIG).
- Produodopa - foslevodopa-foscarbidopa – a continuous infusion under the skin.
When thinking about starting one of these treatments, your Parkinson’s doctor will consider several things like your symptoms, other health issues, and what you prefer.
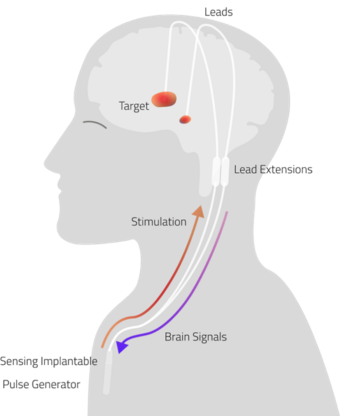
Deep Brain Stimulation surgery (DBS)
DBS is the main surgery used to treat Parkinson’s. It is a well-established treatment which has been used since the 1990’s. The DBS service for Parkinson’s was set up in Bristol 25 years ago. It is one of the largest centres in the UK, treating around 60 new patients every year.
DBS is most effective at improving motor symptoms, such as tremor, slowness of movement, stiffness and dyskinesia. DBS is not a treatment for the non-motor symptoms of Parkinson’s, but it may improve some of them, such as sleep.
How is the device implanted?
In Bristol, this is done under general anaesthesia (you are asleep) with robotic assistance.
- Your head is put in a metal frame to keep it still in the robotic arm.
- Two small holes are drilled in the front part of the skull.
- Small thin tubes called guide tubes are put through the two holes into the brain.
- Thin wires called electrodes are implanted through the guide tubes into the target area in the brain.
- The electrodes are attached to the connecting wires (extension leads). These are placed under the skin and connected to a small battery (similar to a cardiac pacemaker). This is placed beneath the collar bone in a chest pocket.
You will be discharged a day or two after the surgery and return in 4-6 weeks to have the DBS activated once you have healed.
When the pulse generator is switched on, the electrodes stimulate the targeted area in the brain. The stimulation alters signals in the brain to improve the symptoms of Parkinson’s. Over the next 2 years you will have several follow-up visits to adjust the stimulation and your medication.
DBS therapy doesn’t stop your Parkinson's progressing over time. Having DBS may mean you can reduce your Parkinson’s medication by up to 40%, although this is different for each patient. All the DAT options can be useful for people with motor fluctuations, but DBS is the only option that is helpful directly for tremor.
What are the risks?
Like all surgery, there are risks with DBS surgery which include and are not limited to:
- Small risk of infection, especially in the first month. If this happens, you may need to have the DBS removed. You may need to stay in hospital for antibiotics.
- Rare risk of bleeding in the brain.
- Problems with speech and balance, which may improve with re-programming the device.
Who can have DBS?
If you are thinking about DBS, you will have a series of tests to see if you’re suitable for this type of surgery. This may be a day-case or overnight stay and is done by a specialist team, including a Neurologist and DBS Nurse. During the assessment, surgery, and follow-up, you will need to make lots of visits to Southmead hospital. You should think about this when making your decision.
Certain people cannot have DBS, for example if you have a cardiac pacemaker or if you cannot have an MRI scan. Also if you have significant balance or memory problems, then DBS is not suitable. Instead, you may be able to have one of the other therapies on the next few pages.
Apomorphine
Apomorphine is a type of dopamine agonist, like other drugs such as ropinirole, pramipexole and rotigotine. Apomorphine is given subcutaneously (under the skin) using a small plastic cannula connected to a pump. Despite its name, apomorphine is not related to morphine and is not addictive.
Apomorphine can be given in two ways:
- Intermittent injections or “rescue therapy” with and injector pen.
- Continuous infusion using a pump.
Apomorphine can improve movement symptoms within 5-10 minutes. The effect of a single injection usually lasts for about an hour.
Some patients use injections every so often, whilst others need a continuous infusion. Apomorphine infusions are usually given throughout the day but can also be continued overnight in some patients. Apomorphine does not replace most other Parkinson’s medications and needs to be used with them. The infusion must be set up daily and you will be given training and ongoing support with this by a specialist nurse.
Who can have apomorphine?
If apomorphine is being considered, your Parkinson’s specialist will usually refer you to your local apomorphine nurse. You can discuss the therapy in more detail and sometimes arrange a response test. This is done to see if you respond well to the treatment and to check if you have any side effects. You will need to have an ECG and blood tests before the response test.
Your Parkinson’s specialist will not recommend apomorphine if you have problems with low blood pressure, hallucinations, or psychosis, as these can be made worse by the treatment. It may also not be recommended if you have had certain side effects from other dopamine agonists, including impulsive behaviour.
Nausea and vomiting are common side effects when starting apomorphine. An anti-sickness medication (domperidone) is prescribed at the beginning to help with this. Another common issue can be skin reactions, particularly with continuous infusions but these can usually be managed with advice from your apomorphine nurse.
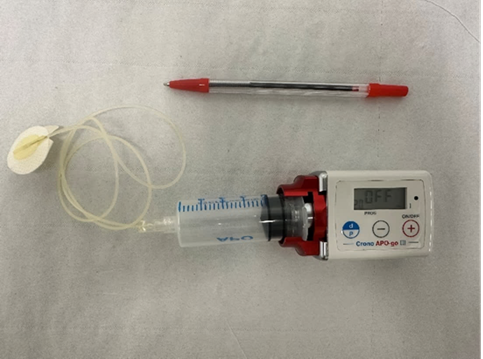
Apomorphine pump
Pen for size reference.
Apomorphine pen
Pen for size reference.

Duodopa: Levodopa-Carbidopa Intestinal Gel (LCIG)
Duodopa is a gel form of the drug levodopa (the main treatment for Parkinson’s). It is delivered directly into the small intestine via a small pump.
This treatment is given through a tube called a gastrostomy or PEG-J tube which needs to be inserted to deliver the gel medication. Patients starting on LCIG are usually admitted to hospital for around 5 days, which allows the gastrostomy tube to be put in. The medication is then started and adjusted to control symptoms. This is overseen closely by a specialist team, including a neurologist and specialist nurse.
The treatment usually runs through the day and replaces most tablet medication for Parkinson’s, except those used overnight. The pump needs to be set up daily and often people need support with this. For some patients, an overnight pump can be added to treat symptoms at night.
We will usually only recommend Duodopa if DBS or apomorphine are not suitable.
What are the risks?
- When the PEG-J is inserted there can be infection and bleeding.
- When the treatment has started there can be:
- Infection around the tube.
- The tube can be blocked or move out of place which stops treatment working. This may mean you need to take tablets again until the tube is unblocked or or replaced (you may need to stay in hospital).
- You may develop a B12 deficiency when taking Duodopa. We will give you a B12 supplement to stop this.
If you are thinking about LCIG, you will first need some tests to see if you’re suitable. This may be a day-case or overnight stay and is done by a specialist team, including a Neurologist and Specialist Nurse.
LCIG pump
Pen for size reference.

Lecigon: Levodopa-Carbidopa-Entacapone Intestinal Gel (LECIG)
Lecigon is another form of levodopa gel treatment. It is similar to Duodopa but has an additional drug called entacapone. This makes the levodopa work for longer. Lecigon became available for the treatment of Parkinson’s in the UK in 2025, but it has been used for several years in other countries.
Like Duodopa, Lecigon requires insertion of a gastrostomy tube. This allows the gel medication to be given directly into the small intestine via a pump. Because the entacapone is added, a smaller amount of gel is needed to control symptoms. This means the pump is smaller and more portable.
What are the risks or side effects?
- Diarrhoea – this may mean you cannot use Lecigon. You may need a trial of entacapone tablets first to see if you can tolerate this,
- When the PEG-J is inserted, there can be infection and bleeding.
- When treatment has started there can be:
- Infection around the tube.
- The tube can be blocked or move out of place which stops treatment working. This means you may need to take tablets again until the tube is unblocked or replaced (you may need to stay in hospital).
- You may develop a B12 deficiency when taking Lecigon. We will give you a B12 supplement to stop this.
We will usually only recommend Lecigon if you are not suitable for DBS or apomorphine.
If you are thinking about Lecigon, you will first need some tests to see if you’ are suitable for this type of treatment. This may be a day-case or overnight stay and is done by a specialist team, including a neurologist and specialist nurse.
LECIG pump

Produodopa: foslevodopa-foscarbidopa
Produodopa is a new treatment for Parkinson’s and was approved by for use in the UK in 2024. Produodopa is a liquid form of levodopa (the main treatment for Parkinson’s) and is given subcutaneously (under the skin), using a pump, the same way as apomorphine.
This pump treatment runs for 24 hours a day to control motor symptoms both during the day and night. This means you will need to wear the pump day and night. Produodopa will usually replace most of your other Parkinson’s medications.
If you are thinking about Produodopa, your Parkinson’s specialist will usually refer you to a Produodopa nurse. You can discuss the therapy in more detail and they will show you how to use the pump. You will also have a series of tests to make sure you are suitable for the treatment.
The treatment can be started either during a short stay in hospital (average 2 days) or as a day-case. You will need several visits to adjust the dose after starting treatment, so it is important to be prepared to attend the hospital often in the first month.
What are the risks or side effects?
As this is a new treatment, we are still developing our understanding of the risks/ side effects and benefits of Produodopa. A common issue from clinical trials has been skin reactions, including swelling, inflammation and skin infections. These can be managed with advice and training by Produodopa nurses. Another common issue we have found is difficulty finding the right dose of medication, which is why you may need to come to hospital more often than with other DAT.
We will usually only recommend Produodopa if you are not suitable for DBS or Apomorphine.
Produodopa pump


Summary of DAT
| Feature | DBS | Apomorphine | Duodopa and LECIG | Produodopa |
|---|---|---|---|---|
| How is it given? | Brain surgery | Subcutaneous needle | Gastric port | Subcutaneous needle |
| How is the device worn? | All internal, nothing visible from the outside | Pump carried during the day | Pump carried during the day | Pump carried day and night |
| Daily support needs | None | Daily line changes | Daily port flushing | Daily line changes |
| Need for oral medication | 30-40% reduced | 20% reduced | All meds via pump | All meds via pump |
Useful information
Further information about advanced Parkinson's treatments and therapies from Parkinson's UK: Advanced Parkinson's treatments and therapies | Parkinson's UK
How to contact us
- 0117 414 8266
- movdiscomplextherapiesadmin@nbt.nhs.uk
- Movement Disorder Complex Therapies Service
Bristol Brain Centre
Elgar House
Southmead Hospital
Bristol
BS10 5NB
© North Bristol NHS Trust. This edition published November 2025. Review due November 2028. NBT003813
Support your local hospital charity

See the impact we make across our hospitals and how you can be a part of it.

