What is a Thyroid Gland?
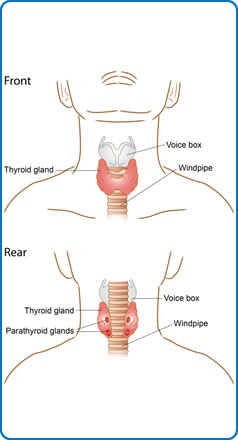
The thyroid is a small gland, shaped like a butterfly, which sits in front of your windpipe in your neck.
What does a Thyroid Gland do?
The thyroid gland secretes a substance called thyroxine. This is a hormone which controls your metabolic rate and so controls your weight and appetite, body temperature and blood pressure and pulse.
What can go wrong that might require an operation? Overactive thyroid (Thyrotoxicosis)
This occurs when the thyroid gland is producing too much of its hormone, thyroxine. This can lead to symptoms such as a fast/irregular heart rate, high blood pressure, weight loss, diarrhoea and anxiety. The treatment of this is usually with drugs but some people may require surgery to remove all of the thyroid gland.
What can go wrong that might require an operation? Goitre
When a thyroid gland becomes enlarged it is called a goitre. This can cause difficulty with swallowing or breathing and may look unsightly. In this situation, an operation to remove half or all of the thyroid gland may be necessary.
What can go wrong that might require an operation? Thyroid tumours
These can be either:
- non cancerous (benign)
- cancerous (malignant)
Growths in the thyroid gland are often first noted as a lump in the neck but can also be found on a scan performed for some other reason or noticed due to “pressure” symptoms in the neck, such as difficulty swallowing or breathing. These are normally investigated with an ultrasound scan in combination with a small needle test (called an FNA). Most of these lumps are not cancerous.
If the needle test confirms a cancer then surgery to remove the entire thyroid gland will be performed. In addition, some of the lymph nodes in the area may also need to be removed.
If the needle test is suspicious for a cancer or is inconclusive, surgery to remove the half of the thyroid gland containing the lump is performed. The sample is then looked at under the microscope. A second operation to remove the rest of the thyroid gland may need to be performed if a cancer is found.
Types of Thyroid Gland operations
The operation performed will depend upon what condition you have and why surgery is being performed. When we meet you in the outpatients department we will ask you about your symptoms and medical history and will review your scans and blood tests. We will then discuss with you the best options for you.
The possible operations include:
- Total thyroidectomy – the entire thyroid is removed. You will need to take tablets to replace the thyroxine that your body can no longer make, for the rest of your life.
- Thyroid lobectomy– only one side of the thyroid gland is removed. In most cases the remaining gland continues to make enough thyroxine for your body. You should have a blood test 6 weeks after your surgery to make sure that do not need to take thyroxine replacement
- Isthmusectomy – occasionally just the middle part of the thyroid gland (the body part of the “butterfly”) needs to be removed
Preparation for Thyroid surgery
Before you undergo surgery you will need to have the following:
- Meeting with a surgeon to discuss your case and make a decision about surgery
- Pre-operative assessment to check that you are fit to undergo an operation. This will include taking a full medical history from you, listening to your heart and lungs and measuring your blood pressure.
- A check of your vocal cords. One of the potential complications of surgery on your thyroid glands is injury to the nerves to your voice box/vocal cords. Therefore, everyone has to undergo a small telescope test up the nose to look down at the vocal cords and check that they are working properly. This takes just a few minutes, and is pain free.
The Thyroid operation itself
To undergo this operation you must first be put to sleep completely, ie. a general anaesthetic. We then make a small incision at the lower part of the front of your neck and perform the operation through this. The type of operation that we perform will have been discussed with you prior to surgery. At the end of the operation we will stitch up your skin with dissolvable stitches so there will be nothing to be removed. We will inject local anaesthetic before you wake up to make you as comfortable as possible.
Possible complications
These can be divided those associated with the actual operation and those with receiving a general anaesthetic.
Surgical:
All cuts in the body can be associated with infection and bleeding
- Infection – this is a fairly quick healing and clean part of the body so infections are not common. However, if your wound becomes red, sore or mucky after you return home then you should contact your GP who can decide if it is infected or not.
- Bleeding – the worst bleeding most patients get is a bit of bruising which resolves with time. Bleeding that requires another operation can happen but is rare. If it does happen, it is usually apparent before you are discharged
- Scar
- Stiff neck – this is fairly common, but usually temporary.
- Nerve injury -there is a nerve that supplies your voice box that runs very near the thyroid glands. This can be injured during the operation, giving you a hoarse voice. This is a temporary problem in 1 in 100 operations and permanent very rarely (1 in 1000 case). Most patients wake up with a sore throat and a hoarse voice from the anaesthetic tube and the surgery so do not worry if this is the case.
- Low calcium levels – Behind the thyroid gland sit 4 parathyroid glands. These control the levels of calcium in your blood and can become injured during thyroid surgery. This results in a low blood calcium level which can cause symptoms such as pins and needles in your fingers/toes and around your mouth. We will be monitoring your blood calcium levels but if you develop any of these symptoms after surgery you should tell a doctor as soon as possible as you may need to take calcium tablets for a short period following thyroid surgery.
- Need for further surgery – In some cases if a cancer is found in the one half of gland removed further surgery to remove the other side will usually be needed.
Anaesthetic:
Possible complications after this operation include:
- Sore throat
- Feeling sick or actually vomiting
- Dizziness from low blood pressure
- Damage to teeth (this is very rare)
You will have an opportunity to talk to the anaesthetist on the day of surgery.
After Thyroid surgery
You need to remain in hospital, usually just overnight. You may experience some pain, but this can usually be well controlled with simple tablet painkillers such as paracetamol and codeine phosphate. You may need to take these for a few days after the operation. Whilst you are in hospital, we will monitor your blood calcium levels. Most patients can go home by lunch time the next day.
At home after Thyroid surgery
Blood tests
You should have your thyroid levels checked with a blood test by your GP about six weeks after your discharge.
Wound care
Your skin will have been closed with dissolvable stitches and covered with a small dressing. This can be easily removed after 3 or 4 days. It is normal for there to be some swelling in the area, which becomes slightly firm. If you are concerned about your wound you should see your GP.
Once the wound is healed over and you are able to comfortably touch your neck you can start to gently massage it E45 Cream or Bio oil.
Pain killers
Most people find that they need to take simple tablet painkillers such as paracetamol and codeine phosphate for a few days after surgery.
Driving
We advise you to avoid driving for a couple of weeks until you can comfortably turn your neck from side to side without any pain.
Talking and Singing
We recommend that you take a couple of weeks off work following this operation. This allows you to rest your voice, with no singing or shouting.
Thyroid surgery follow up
We like to see you in outpatients 2-4 weeks after your operation to check that all has gone well with your recovery. By this stage your thyroid gland will have been looked at under the microscope and we will be able to provide you with more detail about whether you need any further surgery or treatment.
