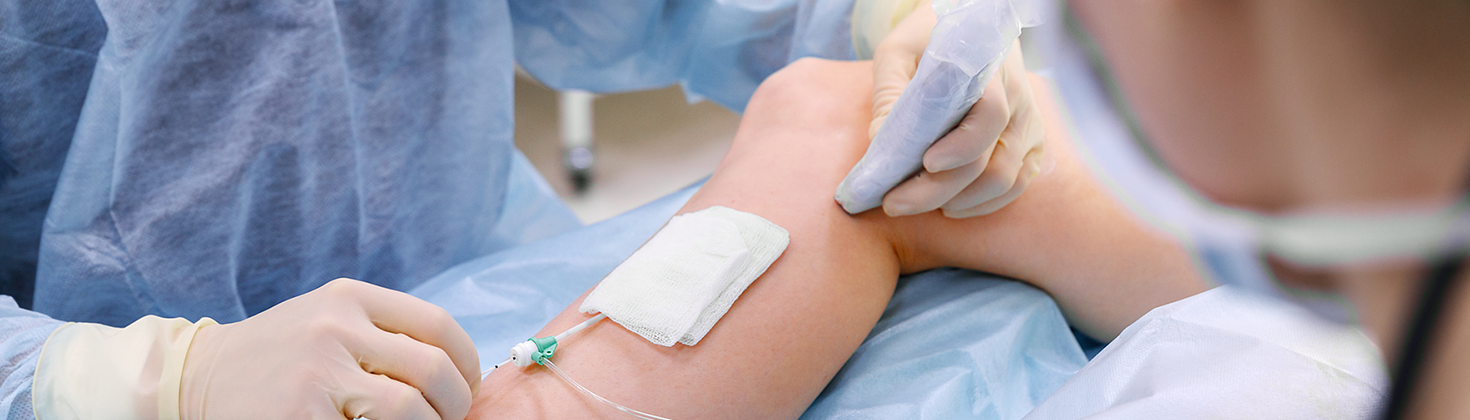
Vascular Current Research
The Vascular Research team conducts research that aims to improve the care of men and women using vascular services department at NBT. This includes arterial surgery, diabetic foot care, leg ulcers, varicose veins, and other vascular diseases.
We have had a successful research team in place for several years delivering complex interventional and observational studies.
The team collaborates widely with other disciplines and professions to develop ground-breaking research and care, for our patients and throughout the NHS.
Please speak to the person treating you to see if there is a research study that may be able to help you.
Current Studies:
CAMELOT
To establish if the use of rectus sheath catheter-delivered local anaesthetic infusion in addition to standard analgesia, is superior to standard analgesia without RSC as defined by the Overall Benefit of Analgesia Score(OBAS)over the first 5 post operative days.
Principal Investigator: Dr Ronelle Mouton / CO-PI Mrs Jane Ashby-Styles
Planned End Date: Recruitment ending 01/05/2026
Local Ref (R&D no): 5126
PLACEMENT
After an amputation, all patients get some pain. Analgesia (pain relieving medicines) help reduce this pain. Managing this pain helps recovery straight after the operation, especially when moving out of the bed with the physiotherapists. The amount of pain felt in the first few days after an amputation may also affect the amount of long-term pain patients get, including “phantom limb” pain. Good pain management is therefore important for every patient.
We are comparing two different types of pain management after a patient has a leg amputation to find out if one method is better than the other.
Project Details
PI: Chris Twine
Planned End date: 31/03/2026
Local Ref: 5365
EADC
The purpose of this study is to evaluate the safety and performance of various Custom-Made Stent-graft Devices (CMD) (this is a tube made specific to the patient’s individual specifications) used for endovascular (inside the vessel) treatment of the main artery of the body (aorta) and related diseases by collecting information on the real-world use of the devices. Health data from at least 600 patients treated at up to 20 hospitals in Europe will be collected as part of this clinical study.
The study results will be used to support the continuation of the CMDs on the market to continue treatment of patients like you. In addition, the study will support the manufacturer’s obligation for post-market product surveillance as well as Cook's technology development.
Project Details
PI: Paul Bevis
Planned End date: 16/09/2030
Local Ref: 5443
EVOCC
Lower limb Peripheral Arterial Disease (PAD) is a form of severe occlusive aorto-iliac disease which affects one in five people over 55 years of age in the UK and is the main cause of leg amputations in the NHS. This is caused by blockages or narrowings in the arteries carrying blood to the leg(s). Some sufferers may develop leg pain when walking whereas others might have leg pain at rest or death of the tissue in the leg(s). This can be leg and life threatening and must be treated with surgery to save the leg or life. The surgery can use one of two common ways of getting more blood to your leg(s):
- Open surgery: this involves an operation to bypass the blocked/narrowed arteries
Endovascular surgery: this involves inflating a balloon inside the blocked/narrowed arteries forcing them to open (angioplasty). Sometimes it is necessary to put a small metal tube into the artery to hold it open (stenting). This type of procedure is called endovascular treatment
Both open and endovascular surgery are currently offered to patients like you in the NHS.
This trial aims to understand which type of surgery is better for saving the legs and lives of patients with PAD, which type is less likely to lead to more surgery in the future and which is better cost-wise for the NHS. If you decide to take part in this trial, you will receive one of the two previously mentioned surgeries and your recovery will be monitored afterwards.
Project Details
PI: Peter Mezes
Planned End date: 01/04/2026
Local Ref: 5524
THRIVE
Endovenous interventions are keyhole operations for varicose veins that are carried out from within the vein itself. Varicose veins are enlarged veins close to the surface of the skin. They are connected to the bigger deeper veins in the leg, known as deep veins. Because of this, operations to close the varicose veins can increase the chance of a blood clot forming in the deep veins. A blood clot in the deep veins (also known as a ‘deep vein thrombosis’ [DVT]), happens in around 1 in 59 people after endovenous operations. A clot in the leg can cause swelling, pain and other problems. If a clot in the leg breaks off and travels to the lungs (called a ‘pulmonary embolism’ [PE]), it may be life threatening.
There is a national drive to reduce blood clots by identifying those most at risk and treating them with medicines that reduce the blood’s tendency to form clots. These medicines are generally very safe but can rarely cause bleeding for example in the bowel and brain. In other short duration procedures, where people can go home on the same day, medicines to reduce blood clots are not prescribed, as developing a blood clot is so rare.
Varicose vein procedures, however, carry a slightly higher risk of blood clot formation, and we are currently unsure if these clot reducing medicines are beneficial in preventing blood clots in patients undergoing these procedures. Elastic stockings or dressings that squeeze the leg and improve the blood flow through the veins are also applied after the varicose vein procedure which helps to reduce the risk of blood clots.
The purpose of this study is to investigate if it is worthwhile prescribing anticoagulants to reduce blood clots after varicose vein procedures. People enrolled in the study will undergo an assessment to make sure that they don’t have the most important risk factors for clots. Those at high risk would not be included in the study. Some participants will receive elastic stockings or dressings alone, while other participants will receive this plus anticoagulation. A computer will decide at random the treatment you will receive.
Project Details
PI: Jude Day
Planned End date: 31/08/2026
Local Ref: 5468
Take Part in Research
Become one of the thousands of people taking part in research every day within the NHS.
About Research & Development

Find out more about our research and how we're working to improve patient care.
Contact Research
Research & Development
North Bristol NHS Trust
Level 3, Learning & Research building
Southmead Hospital
Westbury-on-Trym
Bristol, BS10 5NB
Telephone: 0117 4149330
Email: research@nbt.nhs.uk